MIND YOUR LIVER. IT NEEDS YOU. ™
Alcohol-Associated Liver Disease (ALD) is one of the most common liver conditions. Many people don’t know they have it until it becomes serious.
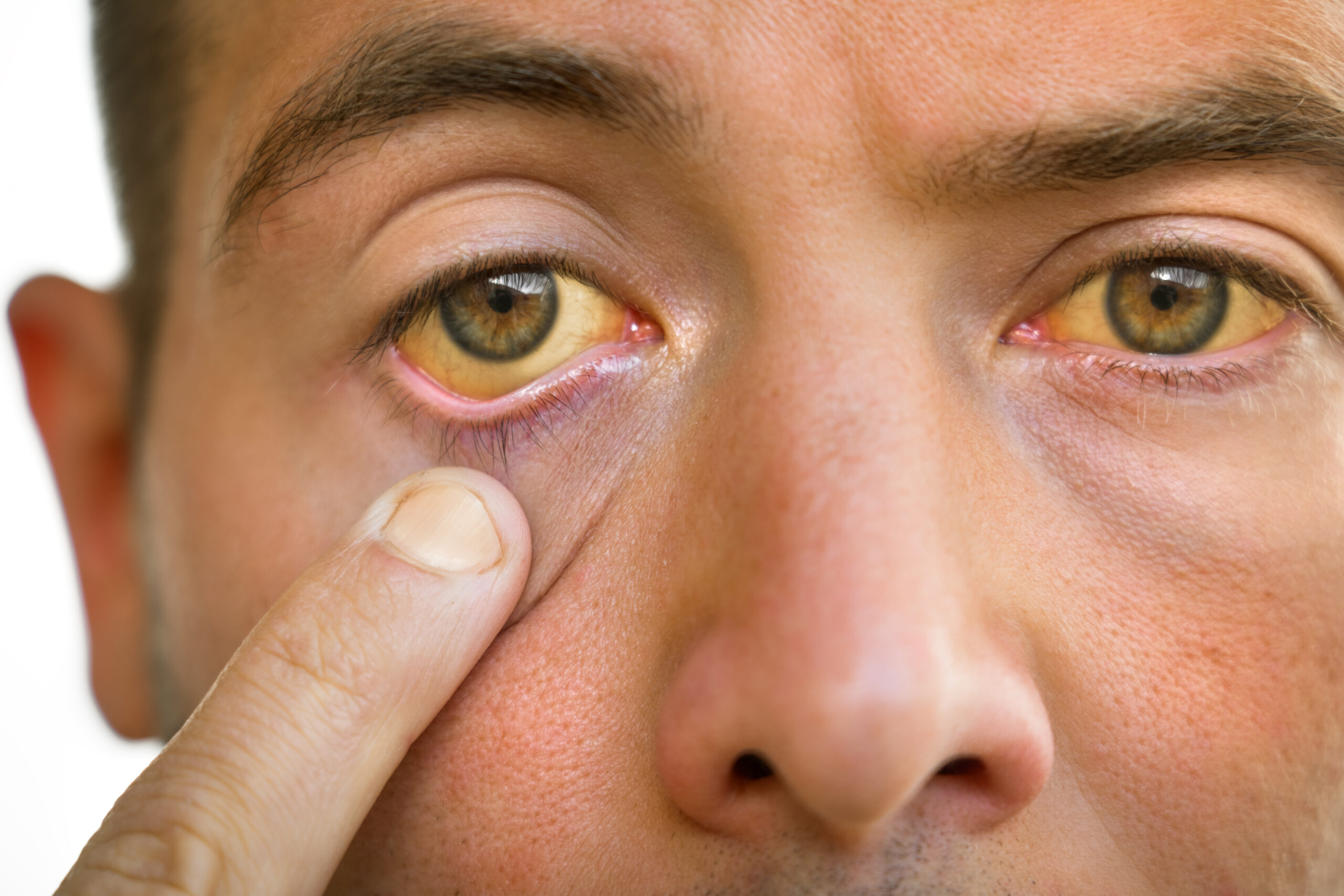
Alcohol-associated liver disease (ALD) is liver damage caused by long-term, excessive alcohol use, including commonly consumed drinks like wine. It can progress from early-stage fatty liver (steatosis) to alcohol-associated hepatitis (inflammation) and, over time, to permanent scarring (cirrhosis).
Early stages often have no symptoms, which is why it can go unnoticed. As the condition progresses, symptoms may include jaundice, fatigue, abdominal swelling, and, in severe cases, liver failure.
Treatment focuses on stopping alcohol use and managing complications early to prevent serious outcomes.
Alcohol associated liver disease can develop gradually over time. Not everyone progresses through these stages in the same way, and some people may move between stages without realizing liver damage is occurring.
This is often the earliest stage of alcohol associated liver disease. Fat begins to build up inside liver cells when the liver becomes overwhelmed and cannot process substances efficiently. Many people experience no symptoms at this stage, which means fatty liver often goes unnoticed. When identified early, liver changes at this stage may be reversible with reduced strain on the liver and appropriate support.
As liver injury continues, inflammation can develop. Alcohol associated hepatitis can range from mild to severe. Some people may experience symptoms such as yellowing of the skin or eyes, discomfort in the upper right abdomen, fatigue, fever, or nausea. In more severe cases, inflammation can become life threatening and requires urgent medical care.
Cirrhosis develops when ongoing liver injury leads to significant scarring and structural changes in the liver. As scar tissue replaces healthy liver tissue, the liver’s ability to function becomes impaired.
In some cases, early or compensated cirrhosis may stabilize or partially improve if the underlying cause is addressed and liver stress is reduced. However, advanced cirrhosis involves permanent scarring and can lead to serious complications, including internal bleeding, fluid buildup, confusion, and liver failure.
Because progression varies widely, early detection and medical care are critical.
Many people with alcohol associated liver disease feel well for years. Because the liver can compensate for damage, symptoms may not appear until significant injury has already occurred. This is why liver disease is often diagnosed later than expected, even in younger adults.
Not everyone experiences every stage, and progression varies based on individual factors and timing.
This page is educational. It’s not a substitute for medical care. If you’re worried about your liver or have symptoms, talk to your provider. You deserve real answers and support.
When alcohol is used in high amounts or frequently, it can lead to fat buildup in the liver (steatosis), inflammation (alcohol-associated hepatitis), and, over time, permanent scarring (cirrhosis).
You binge drink regularly (5+ drinks in one session)
You drink daily or near-daily
Your body has trouble breaking down alcohol due to genetics, liver stress, or other health conditions
Other risk factors can make ALD worse, like poor nutrition, emotional stress, or using alcohol to cope with anxiety or trauma.
Many people have early-stage liver disease and don’t know it. You can feel completely normal, even while your liver is under stress.
But there are signs to watch for:
• Ongoing fatigue
• Mild pain or fullness on the right side of your abdomen
• Yellowing of your eyes or skin (jaundice)
• Easy bruising or bleeding
• Swelling in your legs or abdomen
Bloodwork can show elevated liver enzymes. Imaging tests like ultrasound or FibroScan can detect fat buildup, inflammation, or scarring.
When alcohol reaches the liver, it is broken down into substances that are toxic to liver cells. Over time, this can lead to:
• Fat buildup in the liver (fatty liver)
• Inflammation (alcohol-associated hepatitis)
• Cell damage and scar formation (fibrosis and cirrhosis)
• Disruptions in nutrient processing and immune function
As scar tissue builds, the liver becomes stiff and less able to function properly, affecting how it processes toxins, hormones, and nutrients.
Even small changes in how often or how much you drink can give your liver a chance to heal, especially if you start early.
Set clear limits on how often and how much you drink
Skip binge drinking because it does the most damage in the shortest time
Take alcohol-free breaks, even a few weeks off can help your liver repair
Eat balanced meals, stay hydrated, and fuel your body’s recovery
If cutting back feels hard, talk to a doctor. It is a sign of dependency, not weakness
If you’ve been drinking heavily for years, or notice signs like fatigue, yellowing, swelling, or brain fog, it’s time to check in.
Even if you don’t feel sick, your liver could be under stress.
Getting bloodwork, an ultrasound, or a FibroScan could save your life.
And if you already know you have ALD:
You are not too late.
Stopping drinking can halt or reverse early damage.
You deserve help. No shame, no judgment.
Diagnosis usually involves:
Liver enzyme blood tests (AST, ALT, GGT)
Ultrasound or imaging
FibroScan to check for stiffness and scarring
Liver biopsy in advanced cases
Yes. If caught early and you stop drinking, the liver can heal. Fatty liver and some inflammation are reversible. Stopping alcohol can still save your life.
If your liver is damaged, quitting is strongly recommended. For some, moderation is not safe. A doctor or specialist can help you understand your specific risk.
Binge drinking, even just on weekends, can still cause serious liver harm. It’s about how much and how often.
Genetics, diet, underlying health, and other factors play a role. But if you’re drinking regularly, it’s a risk — and you won’t know how your liver is handling it without tests.
American Association for the Study of Liver Diseases (AASLD)
Practice Guidance: Alcohol-Associated Liver Disease (2020)
https://www.aasld.org
World Health Organization (WHO)
Global status report on alcohol and health 2018
https://www.who.int
National Institute on Alcohol Abuse and Alcoholism (NIAAA)
Alcohol’s Effects on the Liver
https://www.niaaa.nih.gov
We use cookies to improve your experience on our site. By using our site, you consent to cookies.
Manage your cookie preferences below:
Essential cookies enable basic functions and are necessary for the proper function of the website.
You can find more information in our Privacy Policy and Privacy Policy.
